Zee Medical Billing
Revenue Cycle Management Services
At Zee Medical Billing, we offer comprehensive Revenue Cycle Management (RCM) services designed to streamline your billing processes, ensure regulatory compliance, and maximize your revenue. Our dedicated team of experts provides end-to-end support, allowing healthcare providers to focus on delivering exceptional patient care while we handle the complexities of the revenue cycle.
Book An Appointment

99%
Clean Submission

100%
HIPAA Compliance

30%
Revenue Increase

100%
Client Satisfaction
Maximizing Revenue and Efficiency with Zee Medical Billing's Revenue Cycle Management Solutions
Whether it’s a small clinic or a large hospital, all healthcare organizations depend on the smooth coordination of revenue operations to maintain growth and sustainability. And in medical billing healthcare organizations must optimize their revenue cycle management to improve their cash flow, reduce administrative costs, enhance patient satisfaction, and comply with regulatory standards.
RCM can affect every stakeholder, from patients and providers to payers and regulators. That’s why you need Zee Medical Billing which offers unparalleled expertise in healthcare revenue cycle management. We understand the challenges and opportunities of revenue cycle management in the modern healthcare landscape. We offer tailored solutions of medical revenue services from the last two decades in the US that help healthcare organizations boost their revenue, cut their costs, and improve their quality of care
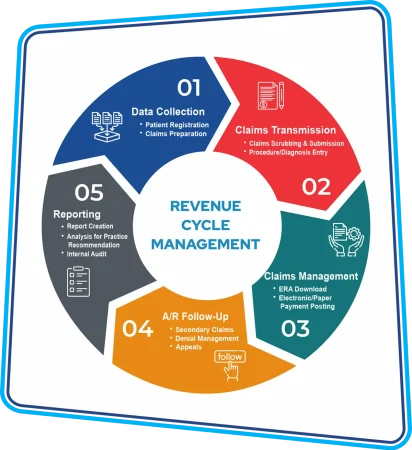
Key Components of Zee Medical Billing's
Revenue Cycle Management Approach
At Zee Medical Billing, we care about your financial health as much as you care about your patients’ health. Our revenue cycle management (RCM) approach covers everything you need to get paid faster and easier. Here’s how we do it:
01
Claims Processing
We simplify the claims processing procedure. From the beginning to the end, we manage your claims using the most recent technology and expertise. We follow up on all claims, examine every detail, and cut down on delays and denials.
02
Timely Follow up
We suggest patient-friendly payment solutions. We know that happy patients are loyal patients. That’s why we offer clear and fair billing practices and flexible payment options. We help your patients pay their bills while helping you collect your revenue.
03
Maximizing Revenue
We strategically generate revenue. We don’t just manage your revenue; we grow it. We identify and address all gaps and opportunities in your revenue cycle using data and analytics. We assist you in finding new sources of revenue and maximizing your current ones
Most Trusted Medical Billing Company in USA
We believe in our services and we would invite you to experience the difference we can make in your net revenue
What RCM Services Zee Medical Billing Offers?
At Zee Medical Billing, we care about your financial health as much as you care about your patients’ health. Our revenue cycle management (RCM) approach covers everything you need to get paid faster and easier. Here’s how we do it:









Our Remarkable Results
20%
Increase revenue by up to 20% through optimized billing processes and reduced claim denials
30%
Speed up your cash flow by 30% by reducing the time your claims stay in AR.
99%
Improve first-pass claim acceptance rate to over 99%, minimizing rework and accelerating revenue.
25%
Expedited reimbursement timelines by 25%, ensuring timely receipt of payments and improved revenue.
50%
Decrease billing errors by 50%, enhancing accuracy and compliance with regulatory standards.
20%
Operational costs were cut down by 70%, driving efficiency and maximizing profitability for healthcare.
Our Clients Achieve Amazing Results

Brian Pervis, N.P
I want to give a great review about ZEE Medical Billing. I have a wonderful experience since I have contract with this company. They are very supportive, very professional and they have helped me increase my revenue. I want to thank ZEE Medical Billing.

Dr. Peter Hsin, MD
ZEE Medical Billing solved the problems we experienced with inhouse billing and cloud-based software used before in order to find the best RCM solution. They have integrity and knowledge for the job. I am happy with my experience and relationship with them.

Dr. Martin McCarthy, PhD
I have been working with ZEE Medical Billing for 4 years. I found their team to be extremely reliable and effective with careful attention to the details. They are extremely courteous and easy to work with. I recommend ZEE without reservation.
FAQ’s
The financial procedures involved in maintaining patient accounts, from arranging appointments to submitting claims and collecting payments, are together referred to as revenue cycle management, or RCM. For healthcare organizations, it is essential since it guarantees effective billing procedures, prompt reimbursement, and stable finances.
Zee Medical Billing offers a full range of RCM services, including revenue analysis, coding and documentation, patient billing, insurance verification, rejection management, and claims processing.
To reduce claim denials and increase revenue recovery, Zee Medical Billing uses proactive denial management techniques. To stop rejections in the future, we examine denial trends, pinpoint the underlying reasons, and put remedial measures in place. Our staff effectively manages the appeals procedure in situations when claims are refused in order to hasten settlement and compensation.
Zee Medical Billing sets itself apart with its knowledge, attentive service, and dedication to client satisfaction. We place a high value on openness, communication, and reactivity to make sure that our clients get specialized solutions that address their unique requirements and objectives.
Numerous healthcare organizations, including as solo practitioners, group practices, clinics, hospitals, and specialized centers, are served by Zee Medical Billing. Regardless of size or specialization, our adaptable RCM solutions are designed to meet the particular demands and specifications of any enterprise.


















